Safe Delivery: Home Birth in Oregon

Courtney Jarecki, a lithe 36-year-old with an earnest gaze and a thoughtful countenance, was as prepared as a woman could be for childbirth when she became pregnant in July 2010.
Jarecki teaches childbirth classes at her business Full Moon’s Daughter and has served as an apprentice at Alma Midwifery, on SE Ankeny Street. Between those two roles, she estimates she’s attended more than 30 births. Perhaps most important, Jarecki believed her body was designed to deliver a baby. She also believed that most women don’t need a hospital or a medical doctor to do it.
When she went into labor in March 2011, Jarecki was sanguine, confident, expectant. Her husband, Dave, filled a birthing tub with warm water in the living room of their Northeast Portland home. When Jarecki began to have back labor—a particularly painful form of labor—she used every technique she knew to cope, including a mantra: Just this one, just this one. “I didn’t pack a bag for the hospital just in case,” she says, “because I was someone who was not going to go to the hospital.”
But Jarecki’s labor did not go as planned. After 54 hours, she saw thick meconium—an infant’s first stool, which can be a sign of fetal distress, especially after a labor as long as hers. So an exhausted Jarecki climbed into the backseat of her minivan and headed for the one place she never thought she would: the hospital.
Given the history of hostilities between hospitals and the home-birth community, many women who choose home-birth remain trepidatious about how they will be received at hospitals. But the doctors and nurses at Legacy Emanuel, where Jarecki transferred, did not look down on her choice to try to deliver at home—this despite what would have been breaches of typical hospital practice, such as letting her labor for two and a half days after her water broke, which could increase a baby’s risk of infection. (The risk of infection is far higher in hospitals than at home, where there are fewer germs.) “To be honest, I was not ready for the kindness that was bestowed upon me,” she says.
Jarecki’s certified nurse midwife—a nurse pratictioner with additional training in midwifery—sat down to talk to her so she could be at eye level. When it became clear that a C-section was necessary to deliver the baby, who was breech, the staff let Jarecki walk to the operating room on her own two feet. Emanuel also granted her every wish: no vitamin K shot, no vaccines. “It was like being at a spa,” she says. “I made a lot of demands, and they honored every one.”
Two hours after she arrived at Emanuel, Jarecki gave birth to a healthy baby girl. She and Dave named her Lazadae, a name she came up with in a dream.
Jarecki’s experience reflects wholesale structural and cultural changes at Legacy Emanuel designed to make the hospital more appealing to women who start delivering at home and to the midwives who help them—thus providing a safe and welcoming alternative when problems arise. Last year some 1,500 Oregon babies were born out-of-hospital, but not every one had a happy ending. Some home-birthers and midwives fail to seek hospital care when a mother or baby may need it—for reasons ranging from fear of reprisal from doctors to some midwives’ lack of experience in recognizing the need for medical assistance. Sometimes this can have serious consequences. Such was the case for Margarita Sheikh, who hired two community midwives (who did not have nursing degrees) to attend her home birth in Eugene in 2011. Eight days after she began laboring, Sheikh, who has said that she repeatedly requested a hospital transfer during her labor, gave birth to a boy with no heartbeat. The boy, Shahzad, was stillborn.
By reaching out to community midwives and bridging the traditional tensions between hospitals and home-birth advocates, Legacy Emanuel hopes to avoid these kinds of tragic scenarios. More than that, Emanuel has gone to great lengths to make its labor and delivery unit more appealing to a growing number of women who want a no- or low-intervention birth in the first place. Initiated in 2006 by the unlikeliest of heroes—a by-the-book, male obstetrician in his fifth decade of doctoring—the program is changing minds, attitudes, and outcomes on both sides of the hospital–home birth divide.
“Home birth is going to happen whether we like it or not,” says Duncan Neilson, chief of Women’s Health Services at all five of Legacy’s hospitals. “Getting mad about it is like getting mad at the rain.”
There is nothing outwardly heroic about Neilson, no broad shoulders, no killer handshake. He’s a self-described introvert and speaks so softly that to record his voice, an iPhone’s microphone must be placed directly in front of him.
Neilson is an obstetrician, though he never intended to be one. His father was an obstetrician. So was his dad’s identical twin. Later, the pair went into private practice together in Portland.
Neilson, who was raised in Northeast Portland and attended Reed College, imagined a career in neurophysiology. And then neuroanatomy. Or human pathology. Delivering babies? Not even a consideration.
And then, just as he was starting his residency at Johns Hopkins and gearing up to pursue a career in academia or research, his wife had their first child. It was 1969, a time when fathers were not allowed in the labor room, but Neilson’s medical credentials earned him an invitation. (Neilson remembers having witnessed only one previous birth—a C-section, which almost caused him to pass out.)
The baby, a boy, was turned the wrong way, so the doctor pulled out a pair of metal forceps, opened them up, and placed them around the baby’s head. “I thought if this goes well, my life will proceed according to plan,” Neilson says. “If not, everything will change.” It was the first time he understood the importance and magnitude of helping a baby enter the world.
In the end, everything did go well (his son, Duncan Neilson III, is the composer-in-residence at the Portland Chamber Orchestra), but the course of Neilson’s life still changed. He became an ob-gyn, and over the next four decades helped literally thousands of women give birth—every one of the babies delivered in a hospital.
During his career, Neilson has seen a lot of changes in how hospitals manage birth, from the 1960s standard practice of having women labor in one room and deliver in another to shifts away from pain medications such as morphine and nitrous oxide. Today epidurals are the norm, and while this kind of anesthetizing allows a woman to participate during the pushing stage of labor, it also requires careful monitoring of her blood pressure. Women with epidurals also must have an IV, and their fetuses’ hearts must be continually monitored in case a drop in pressure affects blood flow to the placenta.
“Now we have this environment that looks like a high-tech intensive-care unit,” Neilson says. “That has caused some people to rebel from the modern obstetrics and seek a return-to-nature kind of approach.”
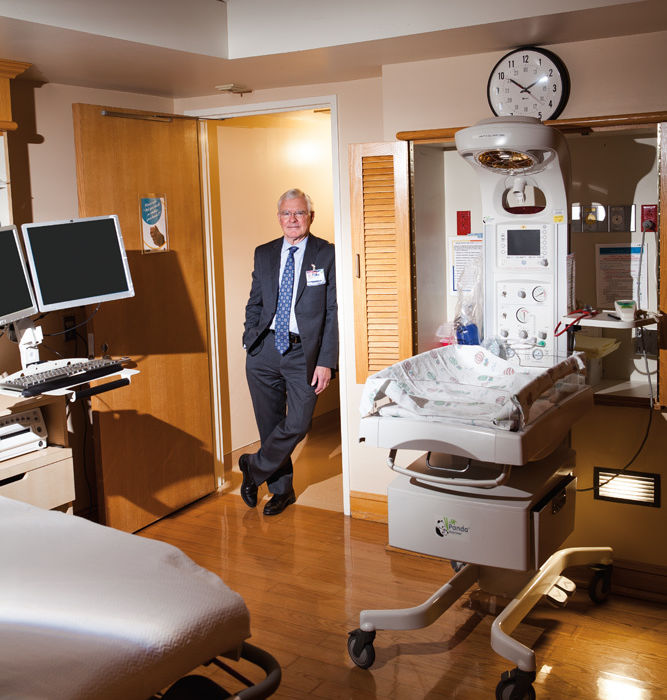
Image: Stuart Mullenberg
Depending on the stats you look at, 2 to 3 percent of Oregon’s newborns take their first breaths in their own homes or at an independent birth center, making Oregon no. 2 in the nation for its rate of out-of-hospital births. (Montana is no. 1.) While such births account for less than 1 percent of babies born in the US, according to the Centers for Disease Control and Prevention they increased 29 percent between 2004 and 2009.
Portland, along with Eugene, Corvallis, Ashland, and Bend, are loci for women who opt to give birth at home. “Midwifery culture goes along with our food culture, our bike culture, and sustainability,” says Holly Scholles, founder of Portland’s Birthingway College of Midwifery, which each year graduates up to nine midwives. “It fits in with that particular Oregonian spirit that combines frontier independence with liberal outlook.”
As more women choose to give birth at home, more women, like Jarecki, will—at some point—need the kinds of services that only a hospital can provide. It isn’t always an emergency that sends them there. Often a woman might be seeking only a labor-inducing drug like Pitocin to move a stalled birth along or an epidural that allows her to rest. Yet in many cases, when hospitals and home-birthers meet, the result can be a savage clash of cultures.
Most obstetricians consider home birth risky at best and reckless at worst. Support for that view: the American College of Obstetricians and Gynecologists reports that out-of-hospital births are associated with a two- to three-times increase in neonatal death, a statistic that is hotly debated. Contributing to physicians’ distrust is the fact that there’s no national standard for midwife licensing; it varies greatly from state to state (except in the case of nurse midwives, who are nurse practicitioners with master’s degrees in nursing plus additional training in midwifery). Oregon has voluntary licensure for midwives who want to be eligible for Medicaid reimbursements.
Most midwives and the women who choose out-of-hospital birth see hospitals as part of a medical system run technologically amok. Support for that view: in 2010, the United States had a C-section rate of some 33 percent, while the World Health Organization recommends that the rates should not be higher than 10 to 15 percent.
And at times, both sides have behaved poorly. “We’ve had midwives who wouldn’t hand over the medical records, because they were so suspicious of us,” says Terri Cohen, the midwifery service program director at Legacy Emanuel.
On the flip side, some hospital staff have been so hostile toward them that some midwives, fearing retribution, have dropped their patients off at the emergency room and fled.
Neilson encountered firsthand the fallout that can occur when home-birth and hospital cultures meet in his first months as chief of Legacy Women’s Health Services. Shortly after accepting the post in 2005, Neilson received a call from a nurse midwife who had overseen a home birth. The mother, who also happened to be a nurse, had had a long and difficult labor. She wanted to come to Legacy Emanuel for an epidural—just to help her rest so that she could continue pushing.
When the attending midwife called the hospital to let staff know they were coming, the obstetrician on the phone—a staunch anti-home-birther—let fly how he felt. “This midwife called me and basically said, ‘What’s wrong with you guys?’ I had to agree that that did not seem like a professional response,” Neilson says.
The experience revealed to Neilson the need for an environment where midwives could safely transfer home-birth patients. “By safe I mean safe from ridicule, and safe from the judgment they were encountering everywhere,” Neilson says.
Neilson, it should be noted, is not an advocate of out-of-hospital birth. He is a fellow of the American College of Obstetricians and Gynecologists and agrees with its most recent statement, issued in February 2011, “that hospitals and [hospital-affiliated] birthing centers are the safest setting for birth ....”
But Neilson possesses an uncommon willingness to look at all of the factors that might be contributing to the midwife-obstetrician divide and arrive at his own, dispassionate conclusions. So he began to ask a question that few other ob-gyns would dare: Does a hospital’s unwelcoming environment to midwives and women who need to transfer prevent them from seeking care when they need it? In short, were the hospitals contributing to poor home-birth outcomes?
“We take care of all kinds of people in hospital who do things that we think aren’t smart. They drink too much, they smoke,” Cohen notes. “But we just don’t tell them they can’t come to our hospital.”
Neilson decided that the right solution was not to condemn the practice, but to turn Legacy Emanuel into a place where women would feel supported, welcomed, and understood. “We wondered, if we create that opening, will they come?”
He was in a position to find out.
Neilson’s first move was to change the way Legacy staffed its labor and delivery floor. Previously, ob-gyns in private practice signed up to work the floor as the on-call delivery doctor one or more times a month—a system that meant the hospital had little control over the attitudes doctors brought with them.
Instead Neilson wanted Legacy Emanuel to hire its own obstetricians, which would give him more say over not just the way they practiced but also their attitudes. “If I said they had to take transfers from community midwives and be nice about it, then they had to do it,” he says. The difficult part was getting Legacy Emanuel to pay for the five doctors’ salaries. But after he argued that in-house obstetricians (called hospitalists) would provide better safety, improve residents’ education, and improve relationships and satisfaction among staff and patients, Legacy Emanuel agreed to lose money on the program. (It costs more to maintain hospitalists rather than rely on on-call docs.)
Up next: changing the protocol for how the hospital handled home-birth transfer patients. Before Neilson’s arrival, all women who transferred to the hospital from home or a birth center were labeled “high risk”—even if a laboring mother only wanted some pain medication. That label meant that home-birth transfers were automatically placed under the care of an obstetrician-gynecologist, rather than, say, one of the hospital’s nurse midwives.
Now, home-birth transfers are assessed individually—often on the phone before a patient even arrives. Obvious emergencies, as when a mother is bleeding heavily, receive immediate care from the staff ob-gyn. Those considered low-risk—about half of the transfers—are placed under the care of Legacy Emanuel’s nurse midwives, who are skilled at supporting natural birth (and empathetic: several, like Cohen, have themselves given birth at home). Before the protocol shift, very few women who transferred to Emanuel from an out-of-hospital birth situation delivered vaginally. Today, about half of them do.
Neilson also wanted to make the hospital more appealing to women who desired a low-intervention birth, in part so more women wouldn’t feel that home birth was their only option for a natural delivery in the first place. He realized water births—common at birth centers and at home—were one of the easiest ways to address concerns about hospitals being “overly medicalized.” When a woman deliveries in a tub of warm water, she can’t have continuous IV infusions and doctors can’t perform continuous fetal monitoring. So in 2008 Legacy Emanuel became one of the first hospitals in Oregon to offer underwater birth. (OHSU has had a water-birth program since 1997, though obstrecians there rarely make use of it. It’s typically used by nurse midwives.)
Since the program at the Legacy hospitals began, some 700 women have delivered babies there using the technique.
As a direct result of the changes Neilson has implemented, Legacy Emanuel is now the go-to place for local midwives whose clients need hospital care. In the first year of these changes, some 30 women transferred to Legacy Emanuel’s nurse midwife practice at some point during their home births; in 2011, that number was 79. The total number of transfers is even greater, when the more emergent cases transferred directly to an OB are taken into account.
“If you make the opening, if you make a more inviting environment, then word will spread,” Cohen says. “We want midwives and women to know that if you are out of hospital and need hospital care, this is good place to bring your patients.”
More important, Neilson says, are what the hospital no longer sees: “We used to have these horrible [home-birth] disasters show up at the ER. And we do not see those disasters now. They have just about gone away.”
Alma Midwifery looks nothing like a hospital. Its birth center is housed in a 1904 Victorian, there is tea in the waiting room, and a candle burns in the foyer when someone is in labor. A great big bathtub anchors each of the four birth rooms, which are decorated with tiled murals, plants, and cute bedsheets. About the only thing that cues a visitor that she is standing in a birthing room and not a bed-and-breakfast is a baby scale.
About 10 percent of the births attended by Alma’s midwives, at the birth center or in mothers’ homes, result in transfer to a local hospital—most of them, if insurance allows, transfer to Legacy Emanuel. The hospital’s willingness to work directly with community midwives has improved care protocols here, says Alma midwife Stephanie Sherman.
As a result of conversations with Legacy Emanuel, Alma changed the way it did its charting. Now, in addition to traditional “story charting”—chronicling the birth with notes about a woman’s family support system, or even the weather—midwives fill out a checklist of vital information on a form prepared by Emanuel’s Cohen to make it easy for doctors accepting transfers to find essential information. “What doctors want to know is What are vital signs for mom? What are vital signs for baby? Is she drinking? When did she last drink?” Alma’s owner and director, Laura Erickson, says.
Alma also prepares its clients better for the possibility of hospital transfer—and even for the possibility of a C-section. “Here it’s not, ‘We’re going to the big bad doctor, the enemy’; it’s ‘We’re going to give you more resources,’” Erickson says. “Hopefully the clients don’t go in with their boxing gloves on and get defensive.”
Alma’s midwives, too, have developed strong relationships with Emanuel’s nurses and the hospitalists—most of whom have visited Alma. Under these kinds of partnerships, women still get to choose how and with whom they give birth, but now the people in charge of their care are working with each other instead of fighting over whose point of view is right.
“The only way we’re going to get to a middle place is by talking about all birth stories and sharing all of the knowledge that both sides have to offer,” says Jarecki, who is coauthoring a book about women’s experiences with home birth.
The result, both Alma’s midwives and Emanuel’s nurses and doctors agree, is a vastly improved experience for the people who count most in the equation: mothers and babies.



