Year of the Nurse: The Heart of Gold
As the battle against Covid-19 rages on, it’s vital to recognize the brave men and women who, every single day, risk their health to protect ours. That’s why Regence BlueCross BlueShield of Oregon is dedicating this special series of articles to eight local and regional nurses who, through their compassion and humanity, have made the difference for thousands of lives.
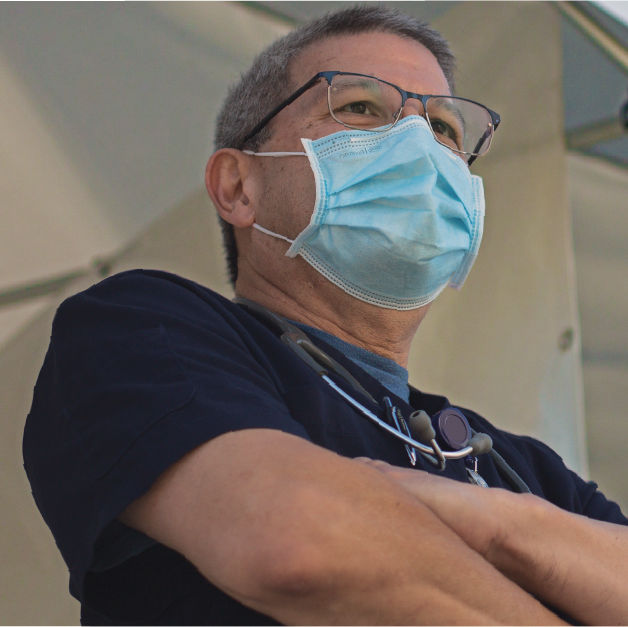
Like some of the hearts she treats at The Oregon Clinic, cardiology nurse Jenifer Ryan’s daily routine was thrown out of rhythm when Covid-19 began to spread. “It was weird the first couple of days,” she says. “Having to stand in line in the morning and get my temperature taken before I could go upstairs. It’s become a habit now, so I don’t even really think about it. It’s funny how fast you adapt to stuff.”

Jenifer Ryan at The Oregon Clinic – Tualatin
Image: Ben McBee
Even as she’s become accustomed to this new reality, she appreciates that the danger coronavirus presents to herself and her patients isn’t going anywhere without a vaccine. The majority of office visitors are older, with underlying health conditions and heart problems, placing them at a higher risk for severe illness due to Covid.
Ryan often assists in procedures where a paper clip–size device called a loop recorder is inserted under the skin to read the patient's heartbeat for up to three years. Generally, these devices are utilized in patients who have passed out or had a stroke, but the causes remain unknown. Under normal circumstances, one of her main responsibilities would be to follow up with that patient, but like most doctor appointments nowadays, that task has gone online.
“Our office has been rapidly trying to find ways to do health care while minimizing their exposure risk. We’ve had some big changes,” she explains. “My wound checks now, I do them virtually. I call the patient, talk to them, and then they put the camera over their incision site. I can see if it doesn’t look infected. I ask them if it feels hot. It can be done.”
Though The Oregon Clinic is doing everything it can to protect its patients, Ryan does know that Covid isn’t just a physical threat; it exacts an emotional toll, too. “The saddest thing I see is all the isolation,” she says. “People in care centers are isolated from their families. They can’t have visitors. They're not out in the halls talking to each other anymore. They’re not eating in the dining rooms. And if they’re elderly and hard of hearing, the phone isn’t the best way to communicate with family.”
It’s a fine line between treatment and prevention, especially when nurses like Ryan are administering cardiac stress tests on the treadmill. “Because of their heavy breathing, if they have something, it’s going to spread a lot further,” she says. “Getting those Covid tests has been challenging.” When the lab they were using ran out, they had to quickly search elsewhere. “We still have to do it though,” she adds, “because we don’t want someone coming in and infecting me, and then I turn around and infect every other patient I see that day.”
There’s growing evidence in the medical field that even people with healthy hearts are experiencing long-term, serious damage from the disease. “There’s a lot of new information that we’re constantly learning,” says Ryan. But wearing a mask, maintaining distance, and washing our hands is the best bet for curbing this pandemic. She adds, “The benefit of reducing the spread is huge, and it’s really not that hard compared to what we’ll gain for our families and our community.”