Comparing COVID-19 Vaccines: Experts Say Don’t Wait
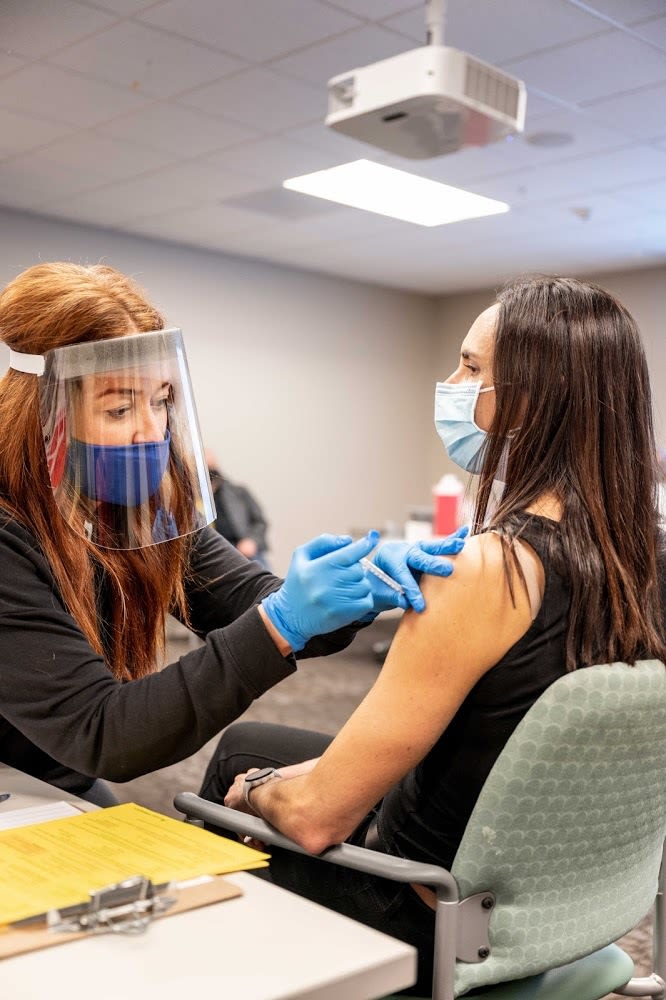
Image: Courtesy Kaiser Permanente
As more COVID-19 vaccines become available, people may wonder if one is better than the others. Reports have even suggested some people are “shopping” for specific brands. However, experts say all three vaccines currently available in the United States are safe and highly effective, and they warn that delaying vaccination to wait for a preferred brand could be risky.
Katie Sharff, MD, an infectious disease specialist with Kaiser Permanente of the Northwest, answers some common questions about how the three vaccines — from Johnson & Johnson, Moderna, and Pfizer — compare and whether people should seek out one over another.
What concerns have people shared when comparing the vaccines?
There is so much focus on the vaccine efficacy numbers that have been reported, but many people don’t understand exactly what those numbers mean. In clinical trials, the Moderna and Pfizer vaccines were shown to be 95% effective, and Johnson & Johnson reported 72% efficacy against moderate to severe disease in the United States. What’s missed in the message is that the Johnson & Johnson vaccine was 100% effective at preventing hospitalization and death after recipients achieved full protection from vaccination. Johnson & Johnson’s is a highly effective vaccine.*
What are the benefits of the Johnson & Johnson vaccine?
The Johnson & Johnson vaccine requires a single dose. Within 14 days of getting the shot, people have built up substantial protection, and after 28 days, they are considered fully vaccinated. By comparison, full protection with the Moderna and Pfizer vaccines requires two doses and takes approximately six weeks. In addition, Johnson & Johnson’s vaccine tends to cause milder and more short-lived side effects. And because it requires only standard refrigeration, it’s easier to distribute in hard-to-reach communities and can be administered in large numbers outside of a specialized clinic.
What’s the problem with waiting for a specific vaccine?
Right now, cases are on the decline, but the coronavirus is still circulating, so every day you aren’t vaccinated is another day you’re at risk. The faster we get people vaccinated, the more we reduce the burden on medical resources and lower the odds of new variants emerging.
How does vaccine hesitancy affect herd immunity?
Herd immunity, also known as community immunity, is reached when enough people have protection against a disease — either by vaccine or natural infection — so that less of the disease is able to circulate. Not only are those people protected, but they indirectly protect those around them who are not yet eligible or who aren’t candidates for the vaccine for other reasons. It’s critical that we get to this level of protection, and the more vaccines we have available, the more opportunities we have to get there.
What else should people know about the COVID-19 vaccines?
Any shot is a good shot. All of the approved vaccines have been thoroughly tested and are safe, effective, and necessary for the safety of our communities. When it’s their turn, people should feel confident taking whichever brand is available. The faster we get communities vaccinated, the faster we can get back to normal life.
=========
Join Dr. Katie Sharff and Portland Monthly for a Facebook Live event at 1 p.m. on March 30, for a Q&A on vaccine safety, vaccine effectiveness, and how taking the shot will protect the health and safety of our communities.
*https://www.cdc.gov/coronavirus/2019-ncov/vaccines/different-vaccines.html