Expert Advice on COVID-19 Vaccines from Kaiser Permanente
Hello, everyone. Welcome. Today, I'm so proud to be here with Kaiser Permanente and Dr. Katie Sharff. I'm Nicole Vogel, the cofounder of Portland Monthly and SagaCity Media, and I want to welcome our guest, Dr. Katie Sharff. She is an infectious disease physician at Kaiser Permanente Northwest. Dr. Sharff has served as KPNW physician lead for influenza for several years and also leads the antibiotics stewardship program. Originally from Portland, Oregon, she attended Williams College in Massachusetts, medical school at the University of Chicago, and completed her residency and fellowship at OHSU. In her free time, she likes to spend time with her husband, two kids, and Berniedoodle—which will always make her smile, we've noticed—and enjoys long-distance running. Welcome, Dr. Sharff. Thank you for being here.
Hi, thanks for having me. I'm excited to be here today.
I think we are all sort of learning everything we can right now about vaccines, and we are so glad to have somebody with your level of expertise. So we'll jump right in to some of the questions that we've seen. Let's talk about efficacy. We keep hearing about the numbers: how effective are the vaccines in use, and if there are differences in the vaccines. Should we have people choosing one vaccine over another?
Yeah, we hear these questions a lot, you know, "When it's my turn, what vaccine should I get? What's the most effective vaccine?" What I want people to hear and the message that I really try to encourage is that right now we have three highly effective vaccines available in the U.S. under emergency use authorization. We have the Moderna vaccine, the Pfizer vaccine, and the Johnson & Johnson vaccine, and all of these vaccines have been shown to be highly effective at preventing disease and preventing hospitalization and death. In the clinical trials in the individuals who received the vaccines, there were no hospitalizations and no deaths in those individuals who received the vaccine. So that's a fantastic vaccine and one that I would encourage you to get—and I would encourage people to get any of the three vaccines that are available to them. As of this point in the U.S., we've given close to 150 million doses, and we're giving upwards of 2.7 million doses a day, but only 28% of our population has received one dose, so we still have a long ways to go in terms of getting to that herd immunity where we have enough people vaccinated to have that protection and get back to kind of normal life—whatever normal is, our new normal.
I'm curious more about that. It sounds like we got some good news about sort of real world instead of just in a test environment—we got some real-world data yesterday. Can you tell us a little bit about that?
Yeah, absolutely. When you look at the clinical trials, for the Pfizer and Moderna vaccines they report around a 95% vaccine efficacy, and then the Johnson & Johnson in the U.S. is around 74% efficacy, so the first thing I want to tell people is not to focus on those numbers. I think there's been way too much media attention to the numbers—you know, 74 versus 95—and like, "Why wouldn't you get the higher number?" Really, it's comparing apples to oranges: the two vaccines were studied at different times in the pandemic, and when you look at the numbers, all of the vaccines are highly effective in preventing hospitalization and death and critical disease. So if a breakthrough infection is feeling fatigued or having a cough—sign me up! I'll take that vaccine.
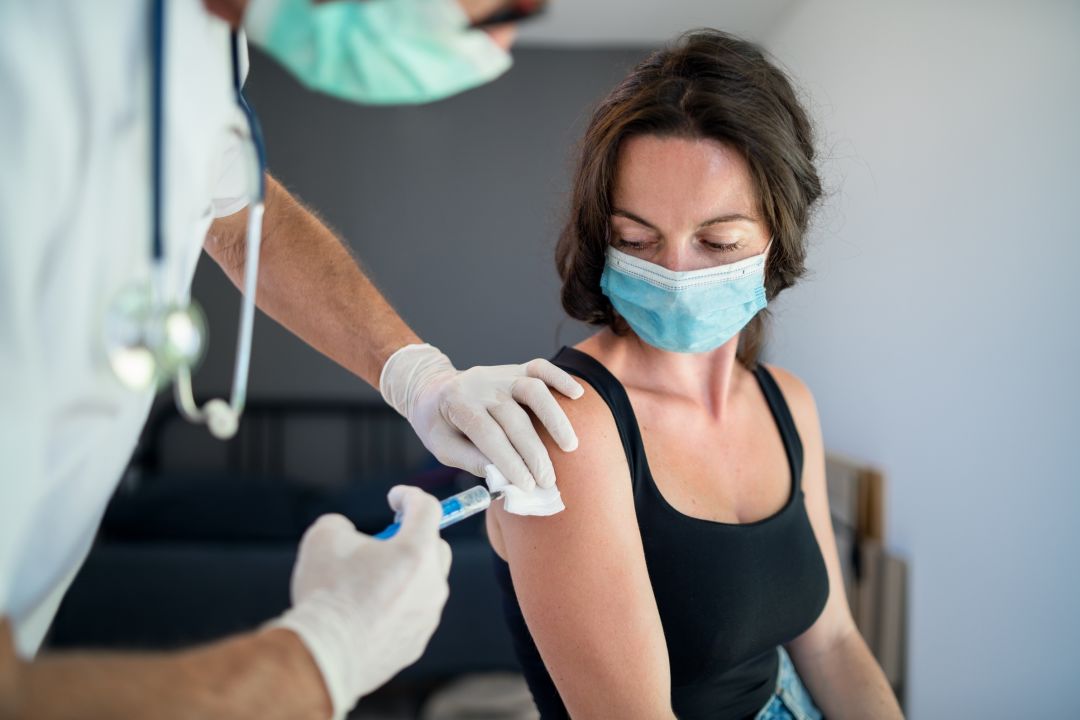
Image: Courtesy Kaiser Permanente
And the data that you're referring to is yesterday, the CDC published some data looking at close to 4,000 health care workers who received vaccines, and they were followed for several months, and showing that that vaccine efficacy that they found in the clinical trials is reproduced in real life. So we have data here in the United States that in real life, these vaccines work, and that's also been shown in Israel as well. So the clinical trials demonstrate the efficacy, and then we have real-life data to really back it up.
Right. And you mentioned Israel—they are now 100% vaccinated as a country? Or they're able to get vaccinated?
I don't know the exact number in terms of Israel's vaccine rate. I know that they've been highly efficient at vaccinating those eligible patients and really had a very organized vaccine campaign, and with that highly effective vaccine campaign have really seen a decrease in their disease incidence. So it goes to show that the vaccine works, and it protects people—yet another reason that here in the U.S., we need to get people vaccinated.
Thank you for that. I think everybody's wondering about the new variants, right? We're hearing about what's happening in Brazil right now, we heard about the U.K. We've also heard that the U.S. has variants that haven't been completely identified. What do we know about the efficacy of the vaccines against those variants?
Good question. So first, I think it's helpful to frame what is a variant, because there's all this, like, "variants, variants, variants"—but what is a variant? What I would say is a variant is to be expected. A variant is just a small mutation in the virus, and that is the natural history of any virus: any virus over time will mutate. It's kind of like when you're transcribing a document, and you make little typos. Those typos are there, and sometimes they have no impact on the document, and sometimes they change it. What matters is if they change the virus.

Image: Courtesy Kaiser Permanente
So that's variants, but then you have to think about: what is a variant of concern? Which is really what we're talking about here. A variant of concern can have one of three properties: (a), it's more contagious; (b), it causes more severe disease; or (c), it doesn't respond to the vaccines, or someone who has previously been infected can get reinfected, so it evades your immune response. In the U.S., the current variant of concern that's of the highest incidence is the B.1.1.7, which fits those first two criteria: it's more contagious, and it causes more severe disease. Thankfully, the data has demonstrated that it doesn't have that third property—our vaccines are truly effective against the B.1.1.7, which is the predominant circulating variant. There are other variants, as you mentioned: the P.1, which is what we've seen in Brazil, and the B.1.351, which originated in South Africa. Those may respond less well to the vaccines. But even so, even if they have a slightly reduced response, what the data has shown is that the vaccines still appear to prevent severe disease, hospitalization, and death.
Really what I want to say is: yes, variants of concern are concerning, but the vaccines that we have appear to protect against the variants. And so I would encourage people to get vaccinated. And I guess the one other thing I would say: we're seeing an increase in cases in the U.S.—I think we had a 16% increase in the last two weeks, probably from the B.1.1.7 variant, which is more contagious and causes more severe disease. And we really, really need to get vaccinated to essentially protect our community so that we don't have these variants circulating unchecked, because as the virus circulates unchecked, it leads to more mutations that cause more concerning variants.
Can you explain that a little bit? How does people not being vaccinated lead to more variants?
So it's really, if people don't get vaccinated, then you just have all of this virus circulating in the community. And as you have more virus, it has the ability to get those typos, to have those little mutations, that then may affect how contagious it is, or how severe a disease it is. As you have more virus out there, it's going to change and mutate and get those little typos, so to speak, that will allow it to mutate and potentially become more severe and more scary for us. So if we can tamp down that virus, we will not only protect ourselves and keep ourselves protected, but we also will reduce the likelihood that we'll have more concerning variants emerging.
So the best thing we can do to keep from more variants is actually to get vaccinated.
Yeah, I mean, I would say: get vaccinated. And then all the things that we've been saying all along: wear your masks, don't gather large groups indoors, socially distance. I mean, those things work. They're simple, but they work. So the things that you've been hearing from public health for a year, plus get vaccinated.
Let's talk about long-term effects of the vaccine. How long do we understand the immunity lasts?
I understand there's a lot of questions about, you know, "How long will I have protection from the vaccine?" And I would say that's a fantastic question. Unfortunately, we don't have a solid answer on that. So what do we know? We know that the vaccines in the clinical trials—in the clinical trial to be approved—it was followed for two months after the last person got vaccinated, but we're still monitoring all of those people who were in the clinical trials. So we have 8, 10 months of data at this point. Do we know how long the protection lasts? At this point, it's uncertain how many months it will last.

Image: Courtesy Kaiser Permanente
I do anticipate that we will need booster shots. So just like you get your flu shot every season, because the flu virus mutates, I anticipate that we'll need to get a COVID booster, whether it's once a year or once every two years—that remains to be seen—but the large pharmaceuticals are already looking at those booster shots to see if they can modify the vaccine to really protect against those more circulating variants. And I think as we get that data, we're enrolling right now here at KP with our relationship for Center for Health Research. As we get that data, then we'll understand the timing of those boosters, but I think it's very likely we'll need booster doses.
Let me ask this. We've seen a lot of people ask the question about long-term effects of the vaccine and whether or not we need to fear the fact that these weren't around a year ago. And so do we know about long-term effects? I've got to believe—with your experience with vaccines across the spectrum from flu—you can give us some comfort about that, or some data.
I completely understand there's a lot of concern about getting these vaccines, because they seem like they were produced rapidly: within a year, we had a vaccine, which is absolutely incredible. And so what I would first start with is telling people that these vaccine platforms—the mRNA vaccines, which is the Pfizer and Moderna, and then the adenovirus vaccine, which is the Johnson & Johnson—these are not new, novel platforms. There have been decades of vaccine research. That's been generated, honestly, by the HIV epidemic, where we've had scientists and researchers in the lab evaluating these vaccines. And because of all of this dedication into vaccine research, where these platforms are used, looking at HIV trials and Zika virus and flu and Ebola, we had these mechanisms, these platforms ready to go to then insert the COVID virus mRNA to generate these vaccines. So it's not some newfangled idea: they've had these for decades.
The other thing I would say is that these vaccines are probably the most scrutinized vaccines in history. They have undergone very rigorous safety and efficacy reviews and are continuing to undergo those reviews. The CDC is continuing to monitor the data: they just looked at, 143 million doses were given last week, and they have found no safety signals. So I would say that these vaccines continue to be evaluated.
And just to clarify, these are not live virus vaccines. There is no active COVID virus in the vaccine. The vaccines give your body the instructions to make that spike protein to protect yourself against COVID-19, but there is no live material. This is not gene therapy; there's no DNA that's in the vaccines. So really, it's a way of giving your body instructions to make that spike protein to essentially tell your body to generate that protection, and then the material rapidly degrades. And for those of you, the spike protein is all those red spikes that we see with the coronavirus—we've seen it so many times—you know, the ball with red spikes. The spike protein is those red spikes, just to clarify.
Speaking of the immune response, talk to us about what people can expect. Certainly people are hearing about side effects to the vaccine. Can you speak a little to that?
Yeah. With regards to side effects, I would say the side effects from these vaccines are what we expect with most vaccines, common side effects being arm pain or swelling at the site of the vaccination. Individuals may have muscle aches, low-grade fevers, headaches, fatigue. Generally, the side effects, if they're going to get side effects, occur one to two days after vaccination. And last, they're short, like a day or two, and then they go away. So really, the side effects, although annoying—you know, you don't feel great, feeling tired and going to work or doing your daily activities—they're short and self-limited. For me, I was actually happy to get side effects, because it's a sign that your body is responding and developing that protection. So I personally had a very sore arm, but was kind of internally celebrating that my arm was sore, because it was a way of telling that my body is protecting me against these vaccines.
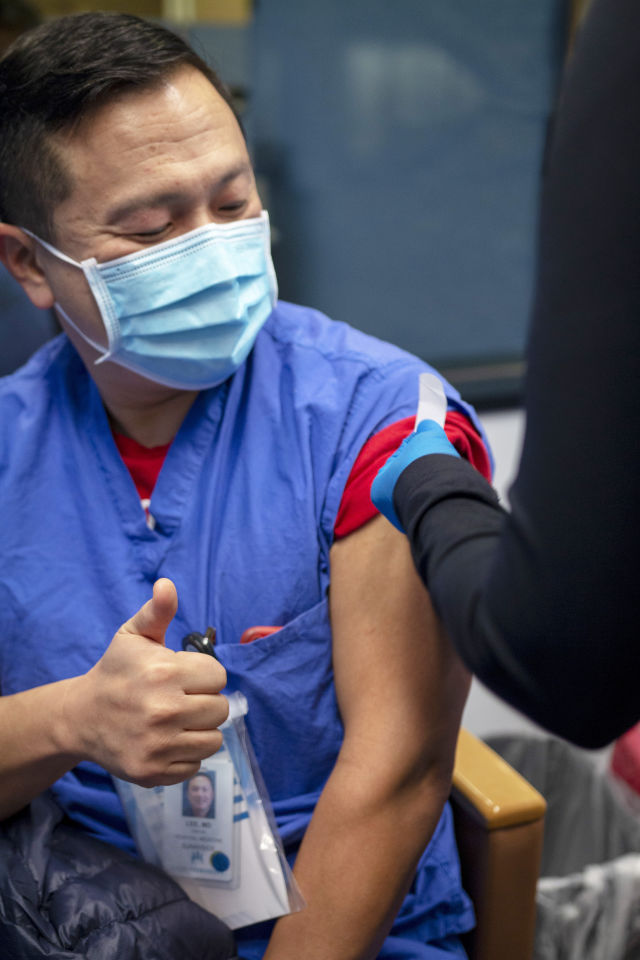
Image: Courtesy Kaiser Permanente
I think there's a lot of questions about allergic reactions; there's a lot of information out there about individuals having allergic reactions. What I would say to that is that with any medication or injection, there's always a risk of allergic reactions. And we know with vaccine—for example, the flu vaccine—the rate of severe allergic reactions is one to two per million doses given. With the COVID vaccines, with the Pfizer and Moderna, the rate they've seen is anywhere from two to five per per million doses given. But what I would say is, these allergic reactions are very recognizable and very treatable and occur after the vaccine is given. When you get your vaccine, you'll be required to either be monitored for 15 minutes, or if you're someone who is more of an allergic-type person, has a history of reactions, 30 minutes. And so if you were to be one of those two in a million that had a reaction, it would be recognized and easily treated. When I think about risks of getting COVID, complications from COVID, long-term complications from COVID, or even dying from COVID versus a very, very, very minor risk of an allergic reaction, I would say, rest assured: these allergic reactions are treatable and very, very rare.
I think a lot of people are talking about, you know, they themselves or friends that are pregnant or planning to become pregnant. What do we know about the vaccine and pregnancy?
Yeah, it's a good question and one that I get asked frequently. Before I talk about the vaccine and pregnancy, I just want to remind people that COVID illness in pregnant women can be very severe. And we know that being pregnant and contracting COVID increases the risk of complication in the mom, increased death in the mom, and an increased risk of preterm labor for the baby. So you don't want to get COVID while pregnant, because it can have very serious outcomes, and we see that.
In terms of the vaccine in pregnancy, pregnant women were not included in the clinical trials for the Moderna, the Pfizer, the Johnson & Johnson vaccine. However, there were individuals who did get pregnant during the trial, and they have not seen any concerning events from that. Additionally, there's been a lot of animal safety data, and we have not seen any concerning events from that. And then we've had tens of thousands of pregnant women who have elected to get the vaccine and are being monitored and not seeing any concerning safety signals from that. So based on what we know about the mechanism of the vaccines, we expect that they will be safe in pregnancy and in lactation. We know that getting COVID while pregnant can be deadly. And so I encourage all of my pregnant and lactating individual patients to get vaccinated because I think: knowing the risk of COVID disease versus some theoretical concerns that we have really no clinical data to back up, I would say get the vaccine. It's going to protect you against COVID illness.
The one other thing, just to follow up, is there was recently a study published that demonstrated that moms who got vaccinated who are breastfeeding actually pass protective antibodies—protective cells—to the baby so that they don't get COVID. So really, another benefit: a breastfeeding mom who got vaccinated is indirectly protecting their baby against COVID.
Great, that's amazing. So the body's doing what it does best, right? I think there's a lot of questions I see out there. One of them is sort of that question that everybody has about: OK, my kids aren't vaccinated, or my grandkids aren't vaccinated, and now I'm vaccinated. What can or should I do around them?
Yeah, it's complicated. And I totally understand: I have two kids of my own, and they ask me when they're going to get vaccinated, even though they hate getting shots. If they're going to take this shot without crying. I'll take it.
Right now, we are not vaccinating children; the studies in adolescents are currently underway. I would say adolescents, which is 12 to 16, we could anticipate maybe end of summer, early fall to be vaccinating, and then the younger children, so 12 and under, they're currently enrolling those kids in the studies. So we're looking at holiday, early 2022 for the young kids—and this is a prediction again, predicting and COVID everything changes, so don't hold me to it, but that's what I'm predicting.
In terms of what you can do, we know that kids who get COVID generally have less severe disease and less complications. So in terms of thinking about, well, can grandma and grandpa who are totally vaccinated come visit our family? We're vaccinated, but the kids aren't. We would say yes, and that's what the CDC is saying. So essentially, fully vaccinated individuals can visit unvaccinated individuals if they're low-risk for severe COVID illness. And so really saying: grandma and grandpa can come over and hang out with the kids, or small gatherings where there are vaccinated adults, there can be unvaccinated children around. We're not at the point where we're going to have large gatherings, weddings, birthday parties with a bunch of unvaccinated individuals. We're just not there yet. I'm hopeful that we'll get there as we get that 70% to 90% vaccination of the population, but we're just not there yet. And with emerging variants, I would say not yet. But grandma and grandpa: definitely come visit the grandchildren.
That is good news, I think, for many of us who have not seen or our kids haven't seen grandma, trying to keep grandma safe. So that's nice to hear. But speaking of eligibility: do you have any sense of rollout and what's happening with number of doses? Clearly, we've made progress, and the U.S. has done a pretty good job compared to maybe Europe. But what are you thinking? And there are a lot of people on this chat who are saying: I'm low priority; when do you think I will get a vaccine? Or when do you anticipate some of those dates will happen for everyone?
A lot of this is coming from the federal government, and then each state has its own prioritization scheme. Oregon is slightly different than Washington, which is different than California. The current administration is saying by May 1, all eligible adults should be able to get vaccinated; we're anticipating a surge in vaccine supply and availability.

Image: Courtesy Kaiser Permanente
So what I would say to people is: we're close. We're close to getting all eligible adults vaccinated. And it's kind of like the light at the end of the tunnel, so I would say: just hold on a little bit longer. Continue to wear masks, and continue to maintain those good safety behaviors—not large gatherings indoors, social distancing, wear your mask—because you're so close, and it would be really, really unfortunate to be days before your vaccine appointment and get COVID. I mean, that's just what you don't want to happen: you're signed up for your appointment, and it's three days away, and then you contract COVID and have severe complications from it. So based on the administration, what they're saying now, we're hoping that all eligible adults: May 1. And then it will take time to get all those shots in arms—that's a lot of people. So I would say, hang in there; you don't want to get COVID. It's kind of the last mile of a marathon: you're so close, we can do this.
This from a long-distance runner—thank you. You know also, people who have had COVID: do you encourage them to get the vaccine, and is there any effect different for them?
It's a great question, the question of: Well, I've had COVID. Should I get vaccinated? And then if I should get vaccinated, what is the timing? What we know and what we recommend is that individuals who have had COVID should indeed get vaccinated, and the reason for that is based on the clinical trial data that getting a vaccine generates a more robust immune reaction than having COVID illness—what we call natural infection. Getting a vaccine, you get more protective response. That being said, we know that in individuals with COVID, generally they're unlikely to get reinfected—at least within the first 90 days, potentially up to several months—and so there's the option to wait. But I generally say if you have the opportunity to get vaccinated, as long as you're asymptomatic and out of your isolation so you've recovered from your COVID, by all means take that opportunity to get vaccinated, because we know that it offers a more robust protection. And as we see this surge and variants and more contagious disease, we really want to have people as protected as possible.
Wonderful. Well, I think that is about all the time we have for today. Sorry I didn't get to everyone's questions; many of them I think you can probably talk to the person who may be giving you the vaccination or your own physician, but we so appreciate your time—that was so illuminating. Thank you so much, and we appreciate everybody's efforts—I know health care work, you guys have been strained a great deal by this, so we appreciate everything that you and Kaiser Permanente have done for our community. So thank you for that, and we hope that everybody got information that was valuable to them, and we look forward to seeing you again soon.
Great. Thank you; take care.
This conversation has been lightly edited for clarity.



