The Truth about Long-Acting Birth Control
Image: Shutterstock
IUDs and implants and shots, oh my! If you’re feeling bamboozled by the myriad birth control options on the market, you’re in luck. We talked to Dr. Carrie Miles MD, MPH of Bridgeview Women’s Health—a Bryn Mawr/Stanford/OHSU-educated obstetrician/gynecologist who currently serves as the Secretary of the Oregon Section of the American College of Obstetricians and Gynecologists’ (ACOG)—to help us break down common misconceptions about long-acting reversible contraception (LARC) methods like intrauterine devices and implants.
You may already be familiar with IUDs; they’re small, T-shaped devices inserted into the uterus to prevent pregnancy. There are currently three types of hormonal IUDs available: Mirena and Lilletta, which both last up to five years, and the smaller Skyla, which lasts up to three. “They all have the same hormone,” Dr. Miles explains. “They just differ in size, hormone dose, and how long they last.” Paragard, the only non-hormonal IUD available, is made with copper and lasts up to 10 years. The contraceptive implant—also considered a LARC—is inserted under the skin in the upper arm and lasts for up to three years.
According to a recent study, LARC use is on the rise: 12 percent of American women choose long-acting reversible contraception, including a whopping 42 percent of women’s healthcare providers. And like many other contraception options, LARC is available for little or no cost through the Affordable Care Act. Still have questions? Read on.
Who would be a good candidate for LARC?
There are very few restrictions for IUD or implant use; in fact, these methods can be safer than other methods like the pill for women with certain medical conditions, such as migraines or high blood pressure. These are great options for women [or anyone with a uterus] who don’t want to have to think about their birth control on a daily, weekly or monthly basis. They can also be helpful for women with heavy and/or painful periods.
Would you recommend IUDs to young women who have never had children?
Yes, absolutely! In fact, ACOG and the American Academy of Pediatrics recommend the IUD and the implant as first-line contraceptive methods for adolescents and young women. Skyla is the smallest IUD and was designed with young women in mind, but really any woman can safely use any of the IUDs.
What about side effects?
Although IUDs differ in the number of years of effectiveness, the key difference for most women is the effect they have on menstrual cycles. The hormonal IUDs and the implant make a woman’s period much lighter and lessen cramps, and some women stop having their period while they are using these methods. Some women love the idea of not having a period, while others may be bothered by not having the monthly reminder that they aren’t pregnant. With the copper IUD, a woman may experience heavier menstrual flow and more intense cramps.
Some women may experience irregular bleeding or spotting with these methods. Most women do not experience mood changes or other bothersome side effects.
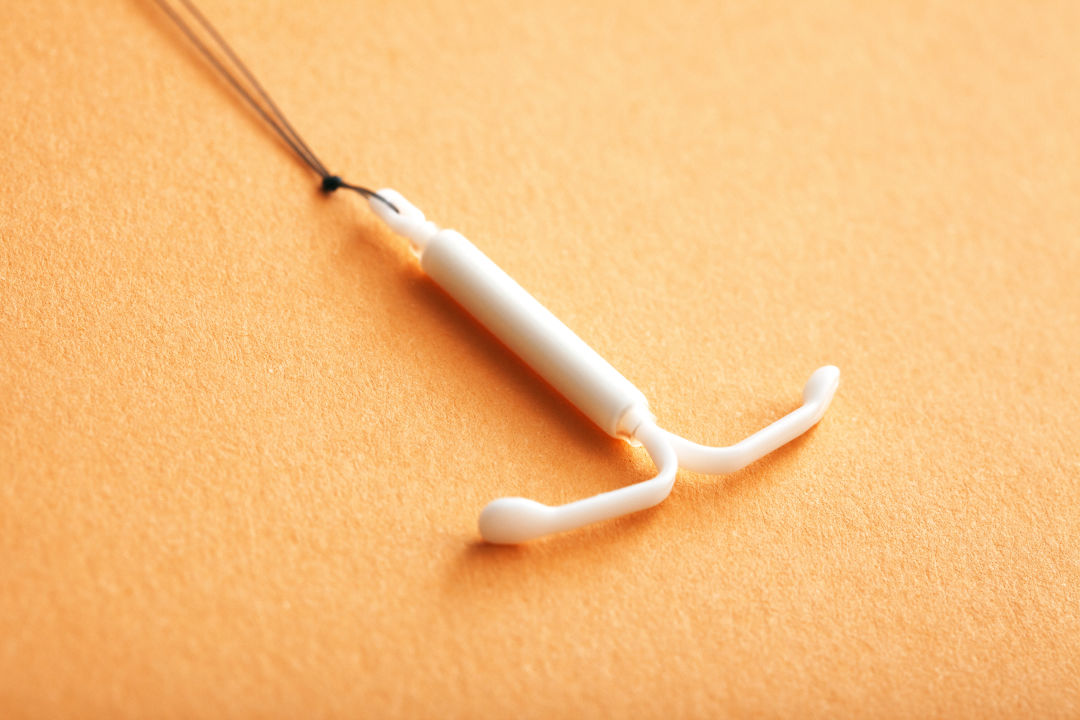
How do the hormonal IUDs work?
All the hormonal IUDs contain levonorgestrel, which is a progestin hormone released centrally in the uterus. Hormonal IUDs have the lowest amount of hormone for any progestin-only birth control—lower than the implant, the “mini” pill, and the injection.
Its main function is to stop sperm in their tracks so they can’t get to the egg. It thickens cervical mucus, which traps sperm. It also makes the lining of the uterus very thin, which is how it helps women who have heavy periods.
What harmful myths exist about IUDs and implants?
The most common misconception is that a woman needs to have had a baby before she can use an IUD. Another myth is that IUDs can cause infertility. There was a specific IUD available many years ago that was unfortunately responsible for pelvic infections and infertility; all the IUDs currently available have been redesigned and do not have any increased risk of infection or adverse effects on fertility.
The main misconception [about the implant] is that it causes weight gain. Though many contraceptive methods can cause a small change in weight, most women don’t see any noticeable change.
What are the efficacy rates of long term birth control compared to more traditional methods, like the pill?
The IUDs and the implant are more than 99 percent effective in preventing pregnancy. They are considered the most effective reversible contraceptives because they don't rely on a woman or couple to use them properly. Other methods, like the pill, patch, ring or injection, have very similar effectiveness if taken correctly and consistently.
Long story short: IUDs and the implant are safe, highly effective, and affordable. If you’re interested, talk to your doctor about your options—and if it doesn’t work for you, they are all reversible.
Oh, and one more thing: If you want to show your IUD pride, this Etsy shop has you covered.



