Why You Need to Get a Pap Smear
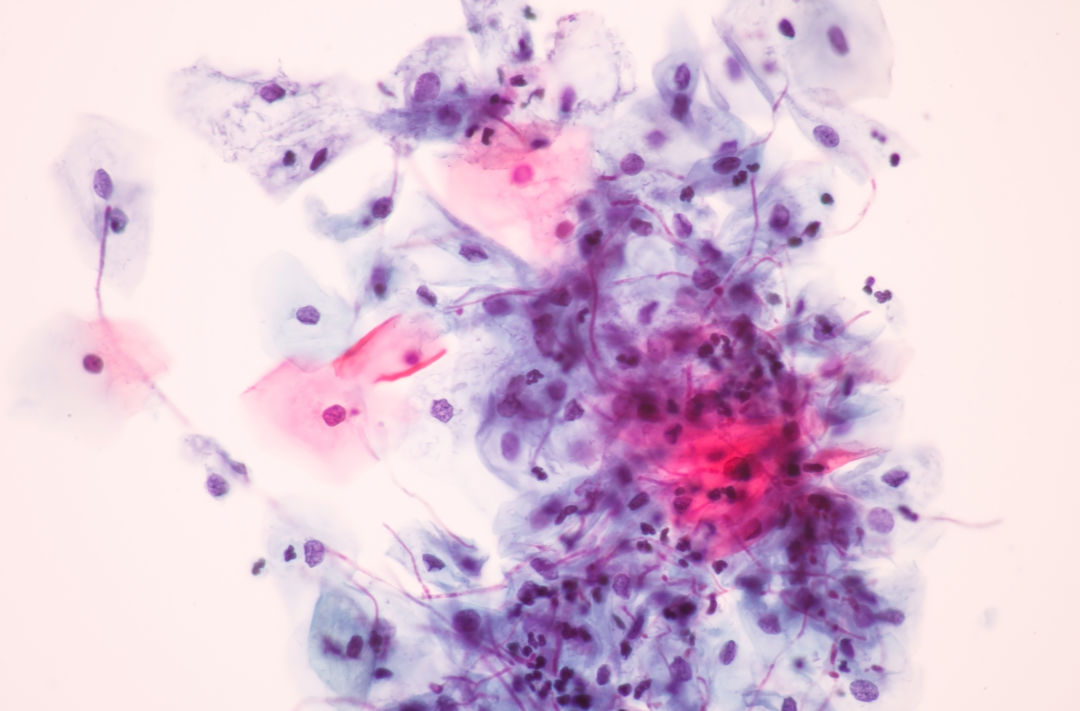
An abnormal Pap smear.
Image: Shutterstock
Lying on a cold exam table, getting a steel speculum shoved deep inside you, and bracing for the dreaded swab may not be high on your list of things to do—but routine pap smears reduce cancer rates and mortality by 80 percent! Guidelines surrounding cervical health are continually evolving, so we sat down with Dr. Robin Barrett, MD, Chair of Obstetrics and Gynecology at Legacy Good Samaritan Hospital, to discuss the current recommendations.
The Notorious P. A. P.
Dr. Barrett recommends getting your first pap smear at 20 years old, and then in 3-year intervals. As long as the pap is normal, gynecologists do not test for the Human Papilloma Virus (HPV)—which causes cervical cancer and genital warts—until patients reach 30. “In young people, the HPV comes and goes, and you get rid of it pretty quickly,” Dr. Barrett explains. “It is very uncommon for HPV to cause cancer in young people.”
The ThinPrep Pap smear has revolutionized pap technology. In the exam room, your gynecologist will take a long swab and scrape off two cell samples: one from outside the cervix and vagina, and the other from inside the cervix. Lab technicians separate the cells from other materials (like blood and mucus), which makes the slide easy to read and improves the odds of detecting precancerous and cancerous cervical cells by a whopping 233 percent, compared to conventional pap smears. During a ThinPrep Pap, your doctor also looks for the high-risk strains (16 and 18) of HPV.
Human Papilloma Virus
HPV is a sexually transmitted virus responsible for almost all cases of cervical cancer. Dr. Barrett claims that there are about 100 known strains of HPV, and that many people will contract the HPV virus but never develop cervical cancer. The original Gardasil vaccine covers HPV strains 16 and 18, and there is a newer version that covers 9 strains. Gardasil is recommended for young people of all genders between the ages of 13–26.
Annual Exams
Dr. Barrett cautions that a pap smear doesn’t take the place of a regular annual exam. During an annual wellness exam, your gynecologist will perform a pelvic and breast exam to look for abnormalities like polyps, fibroids, or cysts. It is also a time to perform STI screenings and discuss sexual health or concerns.
Thanks, Obama!
Don’t forget that all preventative measures and yearly wellness exams are covered under the Affordable Care Act—including mammograms, pap smears, pelvic exams, and Sexually Transmitted Infection (STI) screening.
Other Factors
Exercise, a balanced diet, and abstinence from smoking also impact your chance of developing cervical cancer (and many other forms of cancer). Talk to your healthcare provider about your course of preventative action. The cervical cancer mortality rate has decreased by more than 50 percent over the last 30 years—let’s watch that number continue to plummet.



