This Portland-Based Company Is Helping Non-English Speakers Get Medical Care They Need
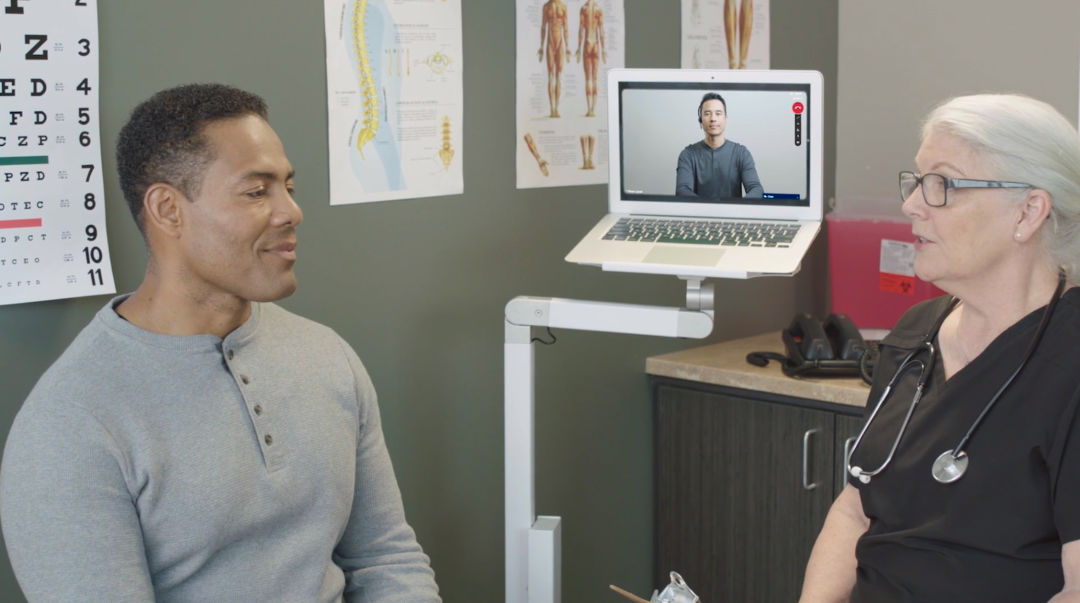
As the medical world shifts toward telemedicine, Portland-based Certified Languages International is hoping to bridge the gap between limited English proficiency (LEP) patients and their doctors.
A few years back, Helen Sweeney and her husband, an English speaking Oregon native, were on vacation in Belarus. Sweeney's husband suffered an infection and had to go to the hospital. The only problem: few doctors in the hospital spoke English. Thankfully, Sweeney speaks Russian and was able to translate for her husband. Being there, and navigating that hospital visit opened Sweeney’s eyes to the importance of medical interpretation, a process by which a trained interpreter passes messages back and forth between patients and doctors. Coupled with the birth of their special needs child, Sweeney turned her more than 20-years of interpreting, mostly in the nonprofit sector, to medical interpretation.
With medical interpretation, Sweeney says interpreters must dedicate themselves to the vast amounts of new information that comes out at rapid speed: new treatments, drugs, procedures, even infectious diseases.
“Case in point, just this year with the entire coronavirus pandemic, that’s a whole new set of work and issues and medical appointments that have been brought into the spotlight,” Sweeney says. “I believe it’s very important for the hospitals and for medical institutions to seek out qualified medical interpreters so communication is as seamless and as transparent as it would have been without the language barrier.”
Since 2018, Sweeney has worked as a Russian interpreter for Certified Languages International (CLI). The Portland-based language services company, which also has an office in Phoenix, Arizona, provides over-the-phone interpreting (OPI), document translation, and video remote interpreting, translating more than 230 languages across the country. (Spanish, Vietnamese, and Russian are CLI’s primary language translations in Oregon.) CLI works with financial institutions and insurance companies, translating for limited English proficiency (LEP), hard of hearing, and deaf individuals, but its focus since founding in 1996 has been in OPI for the medical and health care industry. Its earliest partner was OHSU, which continues to utilize CLI’s language services. CLI also works with the Vancouver Clinic, Legacy, Providence, and other health care providers across Oregon and the US.
When the coronavirus hit the US in early 2020, telehealth services skyrocketed, but Kristin Quinlan, CEO of CLI, says while many health care providers pivoted to include audio-video conferencing (think Zoom, Microsoft Teams, Google Meet, etc.), few accommodated remote-interpreter integration, despite a federal law that mandates any health care provider that receives federal funding or reimbursement provide language services. Not only that, but the Civil Rights Act of 1964 “requires recipients of Federal financial assistance to take reasonable steps to make their programs, services, and activities accessible by eligible persons with limited English proficiency.”
Providing language access for everyone, Quinlan says, is easier said than done. With more than 350 languages spoken in the US, and as the nation still adjusts to the ongoing effects of the coronavirus, Quinlan says this gives health care providers unfortunate leeway to disregard the mandates. More needs to be done, she says.
“As telehealth became a thing and as consumers and physicians alike needed to use it as a result of the shutdown and the pandemic, the consideration for bringing in an interpreter wasn’t there,” Quinlan says. “Imagine not speaking the language and how scary it is, and then not being able to receive services equal to the English population. It’s disproportionately impacted the minority community…. The lack of a solution on telemedicine is really evident and kind of scary.”
To combat this, CLI has been working with hospitals and healthcare providers, creating three-way platforms so providers and patients can bring in interpreters, as well as developing interfaces for more mainstream programs at places such as Walmart. “We’re not going back," Quinlan says of telehealth. “But there is a need for equal access and a need for federal funding. We are looking at unintended consequences. How do we make sure the LEP population is not increasingly more marginalized, particularly considering that COVID is disproportionately affecting the LEP population.”
With the coronavirus’s disproportionate effect on the Latinx community and communities of color, language access and medical interpretation are as important as ever, Sweeney says, and results in better, faster care. Her job, in the age of coronavirus, is not simply passing messages back and forth. It’s evolved into something else.
“It’s different because you are there as a familiar voice. You speak the language they understand,” Sweeney says. “You become also the source of emotional support, even though you’re not necessarily saying anything, but knowing that there’s someone in the room who understands you is priceless—and even if I’m not in the room physically, just on the screen. Knowing that if something is going on, you can say something and you will be heard. I feel like it matters to people more.”
Editor's note: A version of this article appeared in the Winter 2020 issue of Portland Monthly.



