Actual Good News! Norovirus Outbreaks Are Way Down in 2020

Don’t search “vomiting” on Shutterstock. Just don’t do it.
Most “silver linings” of the coronavirus pandemic—more time with the family, upping those baking skills, appreciating the little things—are mere euphemisms for being stuck at home and bored, consumed with existential dread and desperate for distraction. There’s one side effect, though, for which all of humanity can be thankful: the measures taken and behaviors changed to reduce the spread of COVID-19 appear to have brought a steep reduction in outbreaks of norovirus.
“It’s been what I would call a complete and utter nightmare here, of course, dealing with the COVID cases and the wildfires as well, but, yeah, I don’t expect to have any problems with norovirus this year,” says Todd Noble, health director for Linn County, where the entire Albany school district closed for a week in November 2019 to mitigate an outbreak of norovirus.
The highly contagious gastrointestinal nightmare, named after a school outbreak in Norwalk, Ohio, and known for often simultaneous near-liquid diarrhea and vomiting, kills around 900 people in the US in an average year and sickens some 20 million more. It’s largely transmitted through food or contaminated surfaces, or if a sick person’s aerosolized virus particles enter your mouth. In October, when “norovirus season” usually starts ramping up, there were only two outbreaks reported to the CDC by a group of 12 states, including Oregon; in October 2019, there were 66.
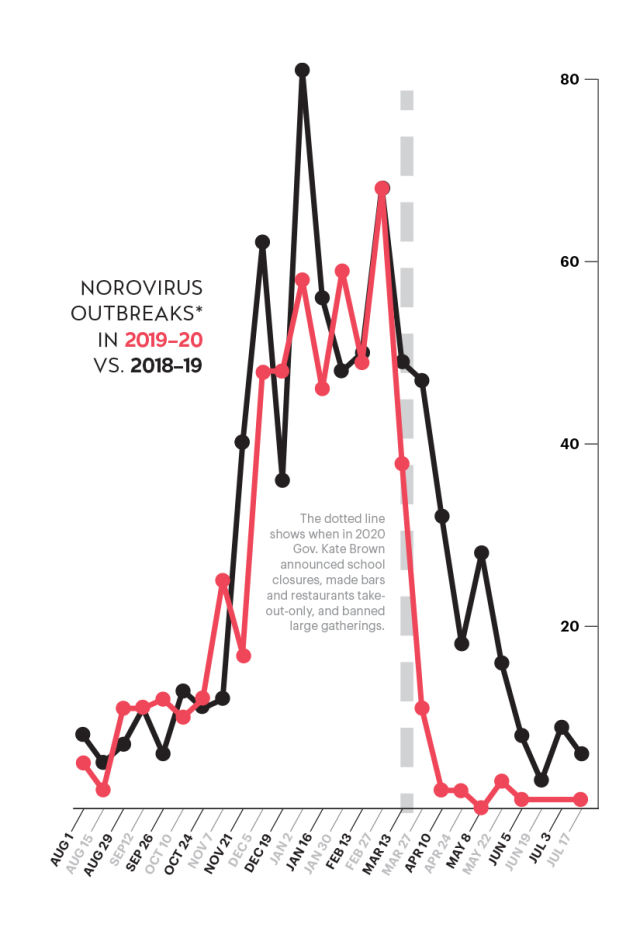
The dotted line shows when in 2020 Gov. Kate Brown announced school closures, made bars and restaurants takeout-only, and banned large gatherings. [*Suspected or confirmed outbreaks reported to CDC via the Norovirus Sentinel Testing and Tracking (NoroSTAT) network by health departments in Massachusetts, Michigan, Minnesota, Nebraska, New Mexico, Ohio, Oregon, South Carolina, Tennessee, Virginia, Wisconsin, and Wyoming]
Image: Michael Novak
“We weren’t sure at first if this was due to social distancing or if it could be explained by underreporting, because we know that a lot of health departments were overwhelmed,” says Dr. Alicia Kraay, a postdoctoral fellow in epidemiology with the Rollins School of Public Health at Emory University in Atlanta. But it does indeed appear that COVID-19 measures, not underreporting or the usual seasonal decline, are responsible for the sudden drop in outbreaks that started in March.
“Probably the biggest driver is just a lot of stuff shut down,” Kraay says, though she notes there were also declines in the size and number of outbreaks in places that couldn’t shut down, like hospitals and nursing homes. “Probably a combination of hygiene, face masks, and distancing seems to have worked,” she says, though it’s hard to conclude what practices specifically made the most difference.
As we enter winter, which usually brings an uptick in norovirus cases, Kraay and her team will keep watching the numbers. Immunity usually lasts about six months after an infection, so the reduced number of cases this year means “we probably have more people that are susceptible,” she says. While that could mean larger outbreaks are ahead, “that’s going to be opposed very strongly by what people are doing with social distancing. What we’re wondering is if maybe the peak will be delayed, if it won’t take off as quickly because it might take a while for transmission to build up in the community.”
For now, though, remote learning, limits on gatherings, attention to personal hygiene and surface disinfecting, and a general sense that it’s our civic duty to stay home if we might be contagious continue to close off a lot of norovirus’s usual pathways to infection. But will these lessons stick?
“Hopefully some of that will spill over,” says Noble, though he warns that hand sanitizer, all the rage amid the novel coronavirus, is not effective against norovirus. A better choice? Good old soap and water.



